New research from the University of Chicago points to microglia, key immune cells in the brain, as a key mediator in the relationship between the gut microbiome and beta-amyloid deposits in male mice in a model of Alzheimer’s disease. The results, published on December 2 in the Journal of Experimental Medicine, indicate that the brain’s immune cells and their connection to our gut microbes may be an important target for preventing and treating dementia in human patients.
The study builds off of previous research showing that perturbations to the gut microbiome, induced by treatment with antibiotics during early life, could reduce some of the hallmark signs of Alzheimer’s disease (AD) in male, but not female, mice.
“Our past work has shown that if you give mice antibiotics beginning shortly after birth, you see a reduction of amyloid deposition specifically in male animals from this particular model of Alzheimer’s disease,” said senior author Sangram Sisodia, PhD, Thomas A. Reynolds Sr. Family Professor of Neurobiology. “In parallel, in the past, we’ve looked at the biology of microglia in the brain and find that in male animals, there are significant changes in the gene expression and morphologies of the cells. In this study, we decided to look at the microglia specifically in the context of this paradigm.”
The study was conducted using APPPS1-21 mice, a popular genetic model of AD. These animals develop pathologies associated with AD, including the amyloid plaques thought to play a central role in the neurodegenerative condition. In contrast to the past work, the new study entailed treating mice with antibiotics for just one week early in life. Even with such a short treatment, the researchers saw a dramatic reduction in in the levels of beta-amyloid in the male brain at 9 weeks of age. Importantly, female mice showed no such differences.
In addition, the research team, led by Hemraj Dodiya, PhD, a postdoctoral fellow in the Sisodia lab, determined that the reduction in amyloid plaques was linked directly to the changes in the gut microbiome by conducting daily fecal matter transplants (FMT) on male mice that had been treated with antibiotics. Restoring the pre-antibiotic microbiome with FMT completely restored the beta-amyloid plaques — it was as if the mice had never been exposed to antibiotics. What’s more, the apparently “neuroprotective” microglia in antibiotics-treated male mice turned into “neurodegenerative”-type microglia with FMT, as if they had never been exposed to antibiotics at all.
“Microglia have a memory,” said Sisodia. “We don’t know exactly what this memory is, but we know that they can respond to a pathogen or perturbation by changing their shape and gene expression and they can sustain those changes for a long time. What we’re seeing in this study is that after antibiotic treatment early in life, amyloid deposition is significantly reduced in males and not in females. And we see that the microglial transcriptome — their gene expression — is changed as well. But if you feed bacteria present in the feces from another untreated mouse to antibiotic-treated mice, you restore the pathology, as well as the microglial phenotype. The final question is, are the microglia responsible for the amyloidosis, and if so, how are the microglia doing this?”
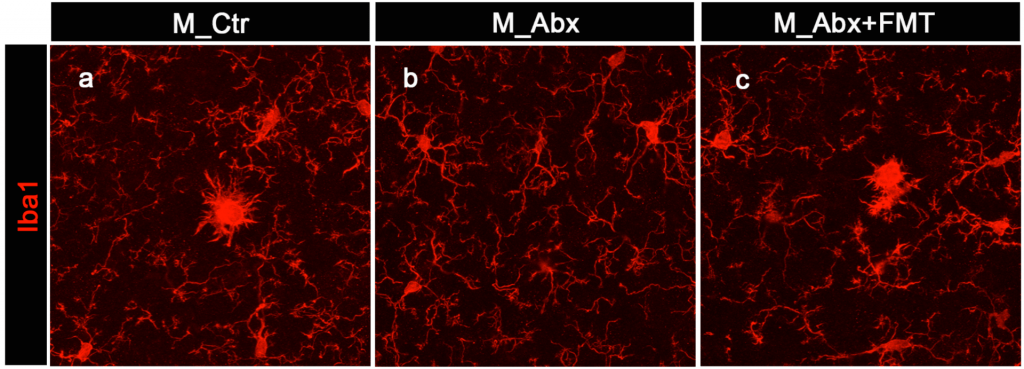
Microglia in the brain of male mice with Alzheimer’s Disease have a “neurodegenerative” appearance and is associated with amyloid beta plaques in the brain (left), while treating the mice with antibiotics early in life leads to “neuroprotective” microglia and reduced amyloidosis (middle). The beneficial effects of antibiotics can be reversed with a simple fecal matter transplant (right).
To answer this question, the researchers gave the mice a drug called PLX5622, which kills microglia in the mouse brain, as well as some peripheral immune cells in the blood stream. They found that without microglia, the antibiotic treatment had no impact on the amyloidosis in the brain, indicating that the microglia are critical for mediating this effect.
“Really, this study shows us three key things,” said first author Dodiya. “The first is that we see these sex-specific changes in amyloidosis in the brain after early life perturbations in the gut microbiome. The second is that simply conducting a fecal matter transplant is enough to restore the amyloidosis after antibiotic treatment, and the third is that the microglia are an essential factor driving the microbiome-initiated changes.”
The research team is conducting further studies that more directly target microglia to ensure the effects of PLX5622 on innate immune cells throughout the body are not affecting amyloidosis in the brain. They hope to clarify what signals the gut is sending to the brain that lead to these changes in the microglia, and how that in turn leads to changes in the amyloid plaques.
The team also is exploring the question of why these effects are only seen in male mice. “It’s an astounding effect,” said Sisodia. “In females, the microglia don’t seem to be affected at all by perturbations in the microbiome. Research in the past has shown that microglia from male and female animals are very different during development and during aging, but what are the contributing factors? It’s likely to be an effect of sex hormones, but then what are the effects on the microbiome?”
Clarifying this question could be important for treating AD in human patients. “Women are at higher risk of Alzheimer’s disease than men, and are usually diagnosed earlier,” said Sisodia. “If we understood what molecules are at play, maybe we could get a better handle on how to go about targeting this disease and why we see these differences between males and females.”
The study, “Gut microbiota-driven brain Ab amyloidosis requires microglia,” was supported by the Cure Alzheimer’s Fund, the Open Philanthropy Project and Good Ventures Foundation, the Bright Focus Foundation Research Fellowship (ID#A2019032F), the Luminescence Foundation and an Alzheimer’s Association Research Fellowship. Additional authors include Ian Q. Weigle, Julia Michalkiewics, Carlos J. Roman-Santiago, Abhinav Srinath, Xulun Zhang, Jessica Xia, Monica Olszewski, Xiaoqiong Zhang, and Eugene Chang of the University of Chicago; Holly L. Lutz and Jack A. Gilbert of the University of California San Diego; Priyam Patel and Matthew John Schipma of Northwestern University; and Can Zhang, Yingxia Liang, and Rudolph E. Tanzi of Harvard Medical School.